Functional Freeze: Why You're 'Bed Rotting' and How to Gently Unfreeze
Author: Dr. Timothy Rubin, PhD in Psychology
Originally Published: April 2026
Last Updated: April 2026

Functional freeze can leave you aware that you want to move but unable to bridge the gap — understanding your nervous system is the first step toward gently coming back online.
Contents
- What Is Functional Freeze?
- Functional Freeze vs. Depression
- "Bed Rotting" — A Cultural Name for an Old Response
- Signs You Might Be in Functional Freeze
- The "Unfreeze Ladder": Coming Back Online Gently
- When Freeze Becomes Chronic
- Why Body and Mind Work Better Together
- A Note on Safety
- FAQ: Functional Freeze and Bed Rotting
You know you should get up. You can see your phone lighting up, your to-do list waiting. But your body feels like it's filled with wet cement. You're not sad, exactly — you're just… offline. If this sounds familiar, you might be experiencing functional freeze — a nervous system response that looks like laziness from the outside but feels like paralysis from the inside.
What Is Functional Freeze?
Most people know about the fight-or-flight response — your body's alarm system when danger shows up. But there's a third survival response that gets far less attention: freeze.
According to polyvagal theory, developed by neuroscientist Stephen Porges, your autonomic nervous system operates across three states. When you feel safe, your ventral vagal system keeps you social and engaged. When threatened, your sympathetic system mobilizes fight or flight. But when the threat feels inescapable or overwhelming, your body defaults to a dorsal vagal shutdown — the freeze response.
This isn't a character flaw. It's an ancient survival mechanism. Just as an animal plays dead when a predator is too close to outrun, your nervous system conserves energy by shutting down non-essential functions. The problem is that in modern life, this response can get triggered by chronic stress, emotional overwhelm, or burnout.
Functional freeze means you're stuck in this shutdown state while still going through the motions of daily life. You might make it to work but feel like you're watching yourself from behind glass. You complete tasks on autopilot but can't remember doing them. You're surviving, but you're not present.
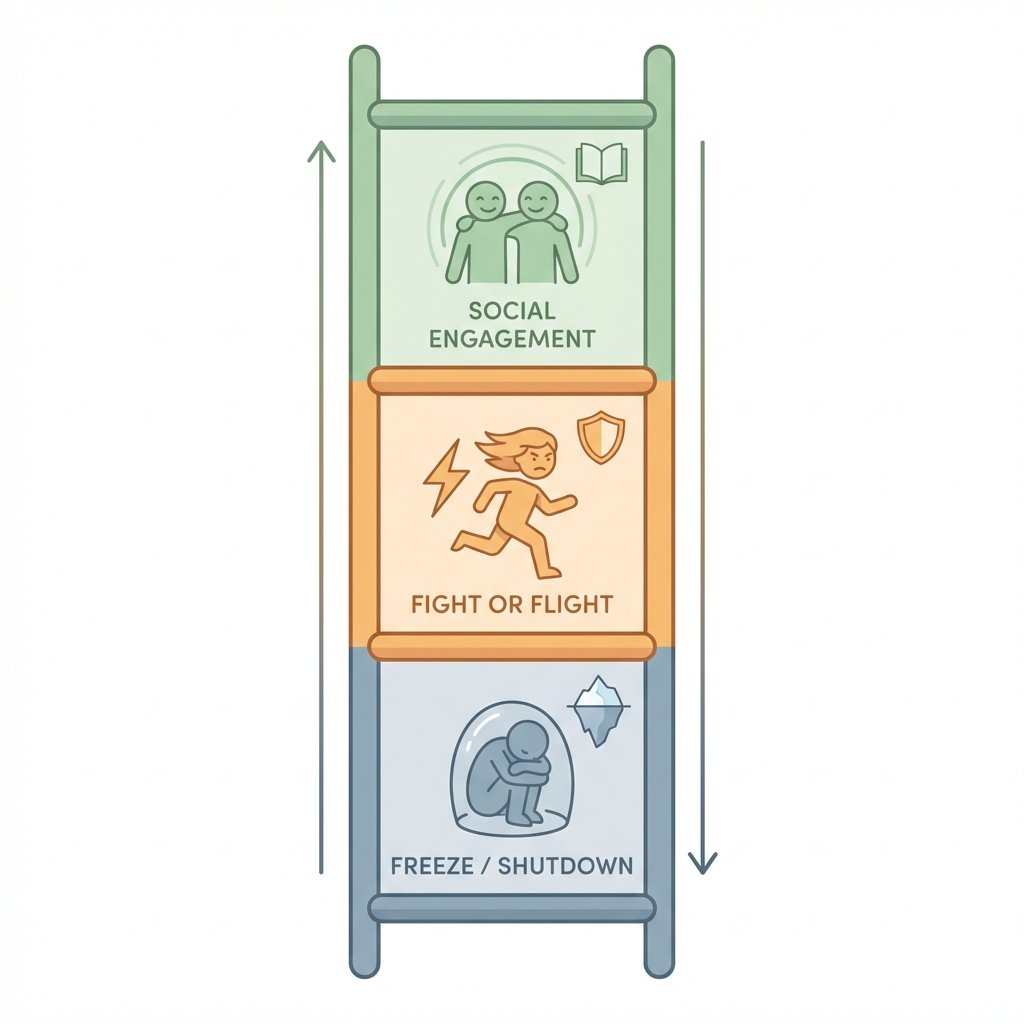
Your nervous system operates across three states — freeze is the shutdown response when overwhelm exceeds your capacity to fight or flee.
Functional Freeze vs. Depression
Freeze and depression can look almost identical from the outside — low energy, withdrawal, difficulty getting things done. But there are meaningful differences.
One hallmark of functional freeze is awareness with inability. You know you want to get up. You can clearly see what needs to happen. But the signal from your brain can't reach your body. Research on dissociative stress responses suggests this reflects a nervous system that has downregulated arousal to protect against overwhelm.
Depression, by contrast, often involves persistent changes in mood, motivation, and self-worth that color your entire experience over weeks or months. With freeze, you may feel completely fine once the response passes — even energized.
Freeze also tends to be episodic and triggered. It often follows sustained stress, emotional overwhelm, or hypervigilance. Depression is more persistent and pervasive. That said, these states can co-occur — chronic freeze can contribute to depressive episodes, and depression can make you more vulnerable to freeze. If you're unsure what you're experiencing, that's a good reason to talk to a professional.
"Bed Rotting" — A Cultural Name for an Old Response
If you've spent time on TikTok, you've likely seen "bed rotting" — the trend of spending an entire day in bed doing essentially nothing. Scrolling, staring at the ceiling, half-watching shows without absorbing them.
Some of this is genuinely healthy rest. In a culture that glorifies productivity, choosing to do nothing can be a legitimate form of recovery. Your body and brain need downtime.
But when bed rotting becomes your default response to stress rather than a conscious choice, it starts to map directly onto the freeze response. You didn't plan to spend four hours in bed, you don't feel rested afterward, and there's a vague sense of guilt mixed with inability to do anything about it.
Research on behavioral withdrawal under chronic stress shows that this kind of disengagement often reflects nervous system dysregulation rather than a preference for rest. Your body isn't choosing comfort — it's conserving energy because it perceives demands as unmanageable.
Signs You Might Be in Functional Freeze
Freeze doesn't always look dramatic. It often shows up in subtle, frustrating ways that are easy to mistake for laziness or lack of willpower.
Mental Signs
You might notice a blankness — like your mind has gone offline. Decision-making feels impossible, not because the choices are hard but because accessing any preference takes enormous effort. You scroll your phone without absorbing anything. You open an app, forget why, and close it.
Studies on cognitive function during dissociative states show that the freeze response genuinely impairs working memory and executive function. You're not imagining the brain fog.
Physical Signs
Your body feels heavy — disproportionately exhausted given your actual activity level. You might notice shallow breathing, physical numbness, or difficulty initiating movement. Even getting out of bed or standing up from the couch feels like it requires enormous effort.
This isn't imagined. The dorsal vagal response actively downregulates metabolic activity, slowing your heart rate and reducing energy availability. Your body is literally in power-save mode.
Emotional Signs
Emotional numbness is a core feature. You're not sad or anxious — you're just nothing. The things that usually bring you joy feel flat. You might describe it as feeling disconnected from your own life, like watching everything through a window.
The "Unfreeze Ladder": Coming Back Online Gently
Here's the most important thing about freeze: you can't think your way out of it. Because freeze is a body-based response driven by your autonomic nervous system, the path out runs through the body first, then the mind. Think of it as climbing a gentle ladder, one rung at a time.

The unfreeze ladder — a gentle, body-first approach to coming back online when your nervous system is stuck in shutdown mode.
Step 1: Micro-Movements
Start absurdly small. Wiggle your toes. Stretch your fingers. Slowly turn your head side to side. These tiny voluntary movements send a signal to your nervous system that you're choosing to move — that you're not actually trapped.
Somatic experiencing research suggests that voluntary micro-movements help shift the nervous system out of dorsal vagal shutdown by reintroducing a sense of agency.
Step 2: Sensory Grounding
Engage your senses with something vivid. Splash cold water on your wrists. Hold something with an interesting texture. Smell something strong like peppermint or coffee grounds.
Sensory input activates your ventral vagal pathway — the branch of your nervous system associated with safety and social engagement. You're giving your nervous system new data: the world out here isn't dangerous. Grounding techniques like these have strong research support for bringing people back to the present moment.
Step 3: Self-Compassion
This step is crucial. The freeze response is often followed by a wave of shame: "What's wrong with me?" That shame activates your threat system all over again, pushing you deeper into freeze.
Self-compassion research consistently shows that treating yourself with kindness during difficult moments reduces stress hormones and supports nervous system recovery. Try placing a hand on your chest and acknowledging: "This is hard right now. My body is trying to protect me." Freeze is a survival response, not a moral failure.
Step 4: One Tiny Action
Not five things. Not your whole to-do list. One thing so small it feels almost pointless. Put one foot on the floor. Open the curtains. Take a sip of water.
The goal isn't productivity — it's breaking the immobility pattern. Each small completed action sends your nervous system a signal: "I can do something, and nothing bad happened."
Step 5: Body-Based Practices
Once you have a little momentum, gentle somatic exercises can help discharge stored stress energy. Try gentle shaking (stand and let your arms tremble loosely), slow rocking, or humming — which directly stimulates your vagus nerve.
Progressive muscle relaxation and body scan meditation are also effective here. They help you reconnect with physical sensations in a controlled, gradual way — essential when freeze has disconnected you from your body.
Step 6: Cognitive Reframing
Once your body is coming back online, then you can engage your thinking mind. This is where approaches like CBT and ACT become useful.
Challenge the narrative that accompanies freeze: "I wasted the whole day," "I'm so lazy," "Everyone else can handle this." These thoughts aren't facts — they're the shame-spiral talking. A more accurate reframe: "My nervous system was overwhelmed, and I'm taking steps to come back online."
When Freeze Becomes Chronic
Occasional freeze responses are a normal part of being human, especially during stressful transitions. But when freeze becomes your default state — lasting days or weeks, interfering with work, relationships, and basic self-care — it's worth seeking professional support.
Research on chronic dorsal vagal activation links prolonged freeze states to conditions like PTSD, complex trauma, and chronic fatigue. A therapist trained in somatic experiencing, EMDR, or polyvagal-informed approaches can help you work with your nervous system in ways self-help may not reach.
Signs it's time to reach out: freeze episodes lasting multiple days, inability to meet basic needs like eating or hygiene, co-occurring feelings of hopelessness, or using substances to cope with numbness.
Why Body and Mind Work Better Together
Traditional talk therapy is powerful — but it's primarily a "top-down" approach, working from thoughts toward emotional change. When you're in freeze, the thinking brain is partially offline. That's why body-based ("bottom-up") approaches are so important.
The most effective recovery from chronic freeze typically combines both. Body-based practices help regulate the nervous system so your brain can come back online. Then cognitive approaches help you process the patterns and stressors that contributed to the freeze.
This isn't either/or — it's both/and. Research on integrated mind-body interventions supports this combined approach for stress-related conditions.
A Note on Safety
If you're experiencing extended periods of freeze, numbness, or disconnection, please don't try to push through it alone. The strategies in this article can help with mild to moderate freeze responses, but they're not a substitute for professional care.
If you're in crisis or having thoughts of self-harm, reach out to the 988 Suicide and Crisis Lifeline (call or text 988) or the Crisis Text Line (text HOME to 741741).
-Tim, Founder of Wellness AI
About the Author
Dr. Timothy Rubin holds a PhD in Psychology with expertise in cognitive science and AI applications in mental health. His research has been published in peer-reviewed psychology and artificial intelligence journals. Dr. Rubin founded Wellness AI to make evidence-based mental health support more accessible through technology.
FAQ: Functional Freeze and Bed Rotting
What does functional freeze mean?
Functional freeze is a nervous system shutdown where you go through the motions of daily life but feel disconnected or unable to fully engage. It's driven by the dorsal vagal response — the same mechanism that causes animals to "play dead."
Is bed rotting a sign of depression?
Not necessarily. Bed rotting often reflects a freeze response triggered by overwhelm rather than persistent low mood. However, chronic bed rotting can contribute to depression over time, so pay attention to patterns.
How long does a freeze response last?
A mild episode may last minutes to hours. Stress-triggered freeze can last a day or two. If freeze persists for weeks and interferes with daily functioning, professional support is recommended.
Can you have freeze and anxiety at the same time?
Yes. Freeze often follows extended anxiety or hypervigilance — when your sympathetic nervous system has been in overdrive too long, it can crash into shutdown. Many people alternate between anxious activation and frozen collapse.
What's the difference between freeze and dissociation?
Freeze is a physiological shutdown; dissociation is the psychological experience of detachment. Freeze often produces dissociative symptoms, but dissociation can also occur without a full freeze response.
Is functional freeze the same as burnout?
They overlap but aren't identical. Burnout is a syndrome of chronic workplace stress. Functional freeze is a nervous system state that can be triggered by burnout, trauma, or any sustained overwhelm.
Why can't I just push through freeze?
Freeze is controlled by your autonomic nervous system, which operates below conscious control. Body-based strategies like movement and sensory input are more effective starting points than willpower alone.
What kind of therapist helps with freeze responses?
Look for therapists trained in somatic experiencing, sensorimotor psychotherapy, EMDR, or polyvagal-informed therapy. These approaches work directly with the body's stress responses.